Up to 20% of all people over the age of 25 are at risk of developing osteoarthritis of the knee. The knee joint works in axial compression mode, therefore its articular surface is subject to constant load and is subject to degenerative changes in the hyaline cartilage.
%20and%20affected%20by%20arthrosis%20(left).jpg)
Prevalence
Pathology of articular cartilage of a degenerative-dystrophic nature with the involvement of bone tissue, articular bags, ligaments and muscles in a process called deforming arthrosis. In terms there are synonyms:
- osteoarthritis;
- osteoarthritis;
- degenerative arthritis;
- arthrosis;
- hypertrophic arthritis;
In terms of frequency, damage to the knee comes immediately after the hip joint, so a stable phrase has been formed: "gonarthrosis of the knee joint". The dependence of disease frequency on age is studied:
| 26 - 44 years old | 5% of adults |
| 45 - 59 years old | 16. 70% |
| 60 - 69 years old | 12. 10% |
| 70 years and above | eleven% |
In all age groups, representatives of the fair sex dominate quantitatively. In it, knee arthrosis occurs 1. 2-1. 4 times more often than in men.
In the field of permanent disability, deforming arthrosis of the knee joint accounts for almost 30% of all causes of disability related to articular pathology.
Classification of gonarthrosis
Due to the development, this disease is divided into two large groups: primary and secondary. Primers arise with no visible preconditions. The secondary is preceded by (or accompanied by) provoking factors:
- biomechanical disorders: injury, overload, developmental anomalies (dysplasia), skeletal pathology (scoliosis, flat feet), obesity;
- inflammatory process: aseptic or infectious arthritis, frequent hemarthrosis in hemophilia;
- metabolic diseases: gout, hemochromatosis, Paget's disease;
- endocrine gland disorders: acromegaly, diabetes mellitus, parathyroid gland disorders;
- violation of adequate blood supply: varicose veins and post-thrombophlebitic syndrome, obliterating endarteritis, atherosclerosis of the vessels of the lower limbs;
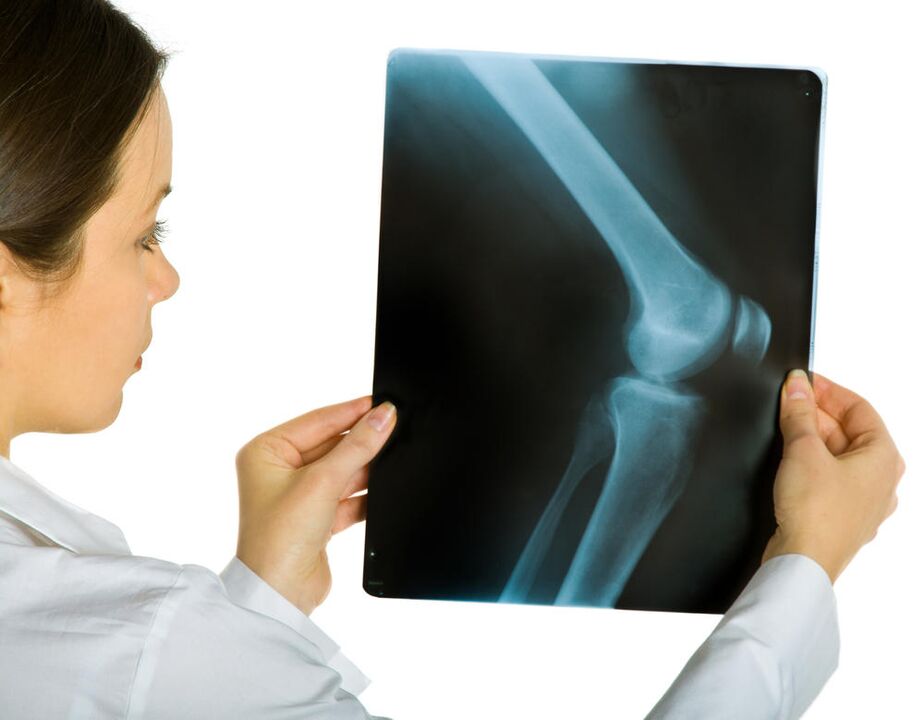
In medical practice, classification according to the severity of pathological changes is more useful. Evaluation is done according to X-ray study. The most popular clinical and radiological classification.
i stage
The picture shows a slight narrowing of the interarticular gap (comparison is made with a healthy joint), the beginning of sclerosis of the pericartilaginous bone tissue. Clinically - pain occurs during walking or immediately after, with prolonged standing. More noticeable when climbing stairs. The pass is at rest. Gonarthrosis stage 1 does not affect joint function much.
level II
The joint space is 2-3 times narrower than usual. Sclerosis is more pronounced, osteophytes are found (spiny growths of bone tissue along the edges of the joint space and condyles). The pain is moderate, there are signs of muscle hypotrophy, lameness. Deformation of the knee on the frontal axis is visible. Gonarthrosis of the 2nd degree leads to significant limitation of joint movement.
Stage III
Sclerosis of cartilaginous elements, deformation of the articular surface. There are areas of subchondral necrosis, local osteoporosis. Cysts in adjacent bone tissue. The joint space is very narrow, sometimes ill-defined. Osteophytes are large in size. Atrophy of the muscles of the thigh and lower leg, the joints are unstable, there are obvious defects. Movement in the knee is sometimes impossible, a contracture is formed. When moving - severe pain, lameness.
This classification approach is convenient because it allows evaluating clinical manifestations in relation to organic changes. It provides an opportunity to choose a more effective treatment based on a comprehensive assessment of the condition of the joint.
Mechanism of development
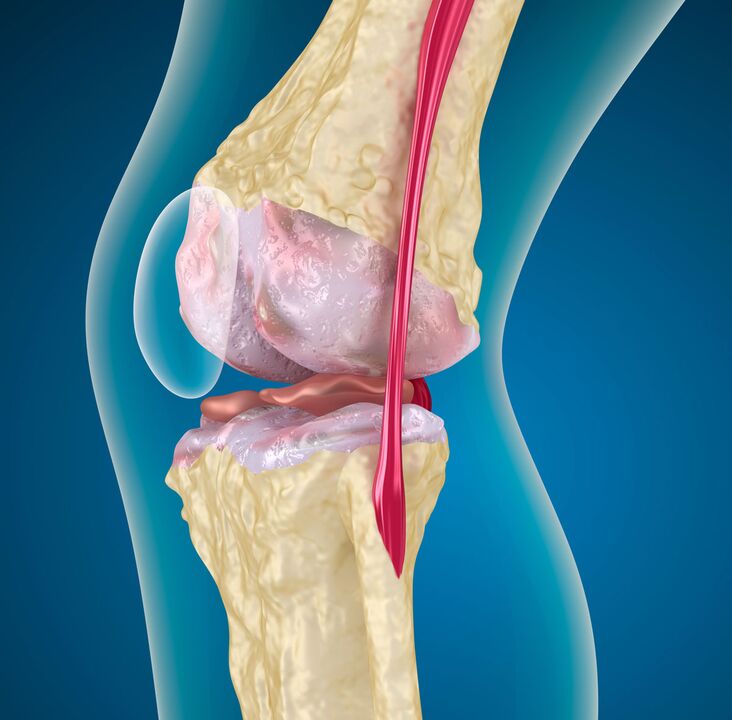
The pathogenesis of any arthrosis goes through three stages:
- Damage to the microstructure of cartilage. Under the influence of any damaging factor, high molecular weight compounds lose their strength and are enriched with water molecules. The ability of low molecular weight collagen to assemble into macromolecules is impaired. This leads to a decrease in the strength and durability of hyaline cartilage. Chondroprotectors overcome such phenomena.
- If the provoking factor is not eliminated, the weakness of cartilage components (glycosaminoglycans, proteoglycans) continues. This leads to the activation of the recovery process. Their power reserve is not that big, so this level quickly passes to the next level.
- Disruption of the compensation mechanism leads to the progressive destruction of articular cartilage, the death of its cells - chondrocytes. Cartilage cracks extend into the underlying bone. The degree of detachment of cartilaginous components increases, their defibration occurs, which leads to the thinning of the hyaline membrane.
On the bone side, with deformed knee joint arthrosis, thickening (sclerosis) occurs, cysts and areas with uneven bone density appear. Therefore, deformation of the articular surface, instability of the joint develops.
Diagnostics
Diagnosis is based on a set of data obtained as a result of survey (anamnesis), medical examination, and instrumental research methods. The latter includes radiographic examination (CT, MRI), radioisotope (scintigraphy), arthroscopy.
Objective examination
It includes the explanation of the patient's life history, the condition before the development of gonarthrosis of the knee joint, collection of complaints and examination. In the process, the presence of provoking factors and the extent of their influence on the development of the disease are explained.
At this stage, it is important to know the condition of the second knee. If you miss bilateral gonarthrosis and focus only on the knee that worries you more, you can make a serious diagnostic mistake.
For this, the functional test should be carried out on two members at once. Attention is paid to pain with active and passive movement, sensitivity to palpation, crepitation (crunching) during extension and flexion. The chronic inflammatory process leads to the appearance of Becker's cyst - the protrusion of the articular bag into the popliteal fossa, which can also be detected by palpation.
Instrumental Method
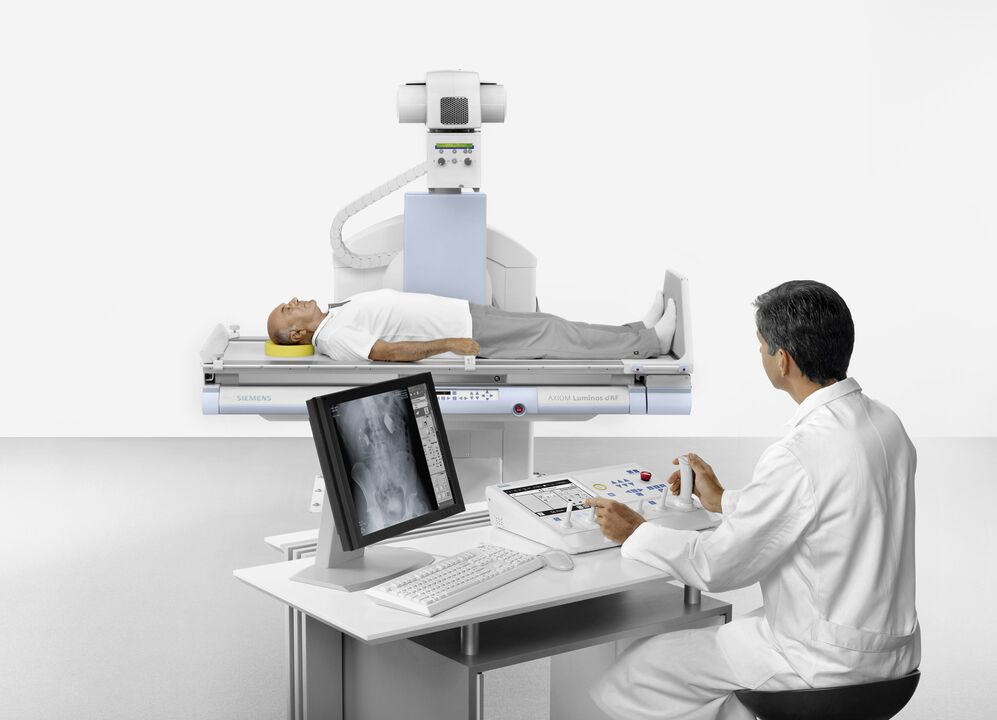
The first is radiography. A picture of the knee in two projections allows an early assessment of the state of the joint and determines the stage of the disease. The disadvantage of this method is that the radiological signs occur later than the symptoms and morphological changes that accompany arthrosis of the knee joint.
In such cases, MRI (magnetic resonance imaging) helps. It is possible to determine the early stages of degenerative changes in the cartilage and bone structure, it is possible to assess the condition of intra-articular ligaments, menisci. Scintigraphy for gonarthrosis of the knee joint provides data on the functional state.
Direct examination of the joint cavity is possible with arthroscopy.
For the consolidation of diagnostic data, the American College of Rheumatology suggests the following criteria:
- Age over 50 years.
- Stiffness in the joints in the morning, which continues for at least half an hour.
- Fractures, determined by movement (active and passive).
If these symptoms are accompanied by osteophytes found on x-rays and pain, it is most likely that gonarthrosis of the knee joint occurs.
The initial stages of this disease may not be expressed, therefore, it is necessary to carry out differential diagnostics with other articular pathologies, where pathogenetic drugs for osteoarthritis (chondroprotectors) will be ineffective.
All possible measures should be taken not to confuse gonarthrosis with the following conditions:
Rheumatoid arthritis |
Onset at an early age, stiffness in the morning for more than 30 minutes, pain worse at rest and weakness in movement, rheumatoid nodules on the skin, concomitant lesions of internal organs, symptoms of intoxication (fever, sweating), C-reactive protein in blood tests. |
Crystal arthritis |
The pain is sharp, at night or in the morning; the skin over the diseased joint is edematous, red, hot; crystals on microscopic examination of synovial fluid, increased uric acid in the blood (with gout). |
Spondyloarthropathies |
Arthritis of other unrelated joints (intercostal, lumbar joints); inflammatory process in the tendon; damage to the cornea, skin, mucous membrane. |
In the International Classification of Diseases of the Tenth Revision (ICD 10), all these diseases are assigned the index "M", but different numerical codes.
This is a fundamentally different pathological process that requires a professional approach to qualified diagnosis and treatment.
Therapeutic measures
If there is a disease, there must be a way to cure arthrosis of the knee joint. And they exist. Help can be provided in many ways.
In the first place is the achievement of traditional medicine, based on an in-depth study of the causes and mechanisms of disease. Medical and surgical methods are used here. Efficient treatment requires the use of drugs, physiotherapy methods and consistent and complex rehabilitation measures.
The second way is treatment with folk remedies. The effectiveness of this method is, to put it mildly, questionable. But they are used, because it is possible to reduce the manifestation of the disease at home. Folk remedies can only be used in addition to drug treatment or as part of complex therapy, it is important to get the consent of the attending physician!
medical assistance
This type of treatment includes the use of various drugs. For medical effects, drugs from different groups are used:
- non-steroidal anti-inflammatory drugs, analgesics, opiates;
- slow-acting symptomatic drugs (chondroprotectors);
- glucocorticoid hormones;
NSAIDs, rapid analgesics, opiates
This group of drugs is designed to eliminate pain. Pain syndrome pretty much spoils the life of patients with arthrosis, its removal significantly improves the quality of human life. NSAIDs, anilides, non-narcotic analgesics and narcotics are able to do this.
A common drawback is side effects. These drugs have a negative effect on the kidneys, the protective mechanism of the gastrointestinal tract. An alternative that can reduce dangerous manifestations is injection. Intramuscular administration damages the stomach less and accelerates the effect.
Because of the side effects, drugs of this group are prescribed during exacerbations, careful selection of the dose is required.
The main advantage of NSAIDs is the many forms for local treatment (ointment, gel). Allows you to control the manifestation of the disease at home.
Analgesics of central action are prescribed for a short period, with the ineffectiveness of the other two groups. The most popular opiates are prescribed during exacerbations, more often with bilateral gonarthrosis. This drug is addictive. You can't take it yourself!
The drug slows down the symptoms
The action of these substances is twofold: they have the ability to reduce pain (as NSAIDs) and contribute to the restoration of hyaline cartilage. Often they are called chondroprotectors.
The effect develops over several weeks (2-8) and continues after cancellation for 2-3 months.
In addition to chondroitin sulfate and glycosaminoglycans, this group includes preparations based on hyaluronic acid, a compound obtained from avocado and soy.
The most studied and popular chondroprotectors (chondroitin sulfate and glycosaminoglycans) are ready-made components of articular cartilage. It is well absorbed into the blood, forming a high concentration in the joint cavity. To accelerate the effect, injections can be made directly into the joint.
It has been proven that chondroitin sulfate, taken in a course of two years at a daily dose of 800 mg, has a stabilizing effect on the joint space in gonarthrosis of the knee joint of the 2nd degree.
Avocado/soy compounds have anti-inflammatory effects. Due to the inhibition of collagenase (decomposing enzyme), they significantly slow down the destruction of cartilage, increasing the synthesis of "their own" collagen. They are also well received.
Hyaluronic acid derivatives are used in the form of intra-articular injections. These funds, like chondroprotectors, improve the functional condition of the knee joint.
The mechanism of action of various drugs of slow symptomatic action is quite different, therefore, their combined use is recommended. A high level of safety allows you to take chondroprotectors for a long time without significant harm to the body.
Glucocorticosteroids
The main action is anti-inflammatory. These funds are prescribed when NSAIDs are ineffective. The tablet form also damages the lining of the stomach. There are forms for intra-articular injection.
They have many side effects, so you should not abuse hormonal drugs for arthrosis deformation of the knee joint.
Group name |
Advantage |
Disability |
|---|---|---|
NSAIDs, analgesics, opiates |
Fast effect, many forms for topical application. |
Side effects, unstable effects, dangerous for age-related patients, addiction occurs. |
Chondroprotectors |
They act pathogenetically, have a lasting effect, are non-toxic, there are forms for external and intra-articular use. |
The slow development of the effect. |
Hormones |
Rapid effect when NSAIDs are insufficient; form for intraarticular administration. |
Side effects, unstable effects, long-term use is impossible. |
ethnoscience

At home, you can reduce the manifestations of the disease with folk remedies. There are many recipes, but there are a few but:
- no clinical studies have been conducted;
- it is impossible to dose the medicinal substance accurately;
- indicators are not clearly defined;
- individual tolerance to folk remedies is not taken into account;
Its advantages include a wide therapeutic range, a large selection for external use. Homemade compresses and tinctures, ointments are popular.
The effectiveness of home treatment can be proven by the fact that biologically active substances (gums, bile, medicinal plant infusions) are used for preparation.
In addition, efficient treatment with folk remedies begins with adherence to diet, weight loss. This method alone, aimed at reducing the load on the joint, can reverse stage 1 osteoarthritis of the knee joint (the condition is young age, sufficient compensatory ability). A healthy diet, in itself, stimulates the body's regenerative abilities. Diet includes: little hunger, vegetables, freshly squeezed juice. It is advisable to add low-fat jelly, jelly to the diet.
External means are very diverse. They mainly have an irritating and warming effect. The most studied components are bile, dimethyl sulfoxide and bischofite. Bile should be used medicinally, and not independently extracted from animal corpses. Dimethyl sulfoxide is an analogue of the chemical warfare agent, mustard gas. Bischofite is an oil derivative. That is the original difference.
All three drugs have an anti-inflammatory effect, however, at home they should be used only after consulting a doctor. These ingredients also have contraindications and application characteristics.
We must not forget the placebo effect in the treatment of folk remedies.
The last thing I want to say is that one has one health. You should not rely entirely on the simplicity and cheapness of folk remedies. If you have already decided to try it, increase your attention to the painful joints. The development of the disease against the background of treatment with folk remedies is a reason to reconsider the therapeutic approach.
If osteoarthritis of the knee joint grade 2 or higher is diagnosed, it is better not to play around with traditional medicine. Or postpone it for a grace period. Unsatisfactory treatment is an indication for complex surgical intervention.
























